ResearchLibrary List

Radiofrequency Ablation for the Treatment of Benign Thyroid Nodules: 10-Year Experience
Longer follow-up after radiofrequency ablation (RFA) of benign thyroid nodules is needed to understand regrowth and other causes of delayed surgery and long-term complications.

From ablation to operation: Unraveling the surgical outcomes and complications of thyroidectomy after radiofrequency ablation
Radiofrequency ablation is a minimally invasive treatment for thyroid nodules; however, concerns exist regarding its impact on subsequent thyroid surgery. We compared surgical outcomes and complications between patients undergoing thyroidectomy after radiofrequency ablation (post-radiofrequency ablation thyroidectomy group) and those without prior radiofrequency ablation (non-radiofrequency ablation thyroidectomy group).

Radiofrequency Ablation as a Minimally Invasive Treatment for Benign Thyroid Nodules: A Clinical Study
While benign thyroid nodules are often asymptomatic, they can cause cosmetic concerns and physical discomfort, leading to the need for treatment. Radiofrequency ablation (RFA) has gained attention as a non-surgical option to reduce nodule size and alleviate symptoms.

Efficacy and Safety: A Multi-institutional Prospective Cohort Study
Radiofrequency ablation (RFA) has been recently adopted into the practice of thyroidology in the United States, although its use as an alternative to traditional thyroid surgery in Asia and Europe came near the turn of the 21st century. In the United States, only a few studies with small sample sizes have been published to date.

Thermal ablation of thyroid nodules: are radiofrequency ablation, microwave ablation and high intensity focused ultrasound equally safe and effective methods?
Objectives: This study compares volume reduction of benign thyroid nodules three months after Radiofrequency Ablation (RFA), Microwave Ablation (MWA) or High Intensity Focused Ultrasound (HIFU) to evaluate which of these methods is the most effective and safe alternative to thyroidectomy or radioiodine therapy. Material and methods: Ninety-four patients (39 male, 55 female) with a total of 118 benign, symptomatic thyroid nodules were divided into three subgroups. HIFU was applied to 14 patients with small nodules.

Is There a Minimum Number of Thyroidectomies a Surgeon Should Perform to Optimize Patient Outcomes?
Objective: To determine the number of total thyroidectomies per surgeon per year associated with the lowest risk of complications. Background: The surgeon volume-outcome association has been established for thyroidectomy; however, a threshold number of cases defining a "high-volume" surgeon remains unclear. Methods: Adults undergoing total thyroidectomy were identified from the Health Care Utilization Project-National Inpatient Sample (1998-2009). Multivariate logistic regression with restricted cubic splines was utilized to examine the association between the number of annual total thyroidectomies per surgeon and risk of complications.

Radiofrequency ablation of benign thyroid nodules: A prospective, multi-institutional North American experience
Radiofrequency ablation for benign thyroid nodules aims to achieve a volume reduction rate of ≥50%. However, factors that predict treatment success have not been defined in a large-scale study.
![Durante C, Grani G, Lamartina L, Filetti S, Mandel SJ, Cooper DS. The Diagnosis and Management of Thyroid Nodules: A Review [published correction appears in JAMA. 2018 Apr 17;319(15):1622. doi: 10.1001/jama.2018.3696.]. JAMA. 2018;319(9):914-924. doi:10.1001/jama.2018.0898](https://static.wixstatic.com/media/e5b602_15f58e44843145bbb181560017d6117a~mv2.jpg/v1/fill/w_265,h_265,al_c,q_80,usm_0.66_1.00_0.01,enc_avif,quality_auto/Image-empty-state.jpg)
diagnosis and management of thyroid nodules: a review
Thyroid nodules are common, being detected in up to 65% of the general population. This is likely due to the increased use of diagnostic imaging for purposes unrelated to the thyroid.

Efficacy and Safety of Radiofrequency Ablation for Benign Thyroid Nodules: A Prospective Multicenter Study
To assess the efficacy and safety of thyroid radiofrequency (RF) ablation for benign thyroid nodules by trained radiologists according to a unified protocol in a multi-center study.

Use of Radiofrequency Ablation in Benign Thyroid Nodules: A Literature Review and Updates
Successful thermal ablation using radiofrequency has been reported in various tumors including liver or kidney tumors. Nonsurgical minimally invasive ablative therapy such as radiofrequency ablation (RFA) has been reported to be a safe and efficient treatment option in managing symptomatic cold thyroid nodules or hyperfunctioning thyroid nodules.

Radiofrequency ablation for treatment of benign thyroid nodules: A PRISMA-compliant systematic review and meta-analysis of outcomes
Background: Thyroid nodules (TNs) usually appearing in the general population have the potential possibility of malignant transformation and common problems of jugular oppression such as dyspnea and hoarseness. We performed this meta-analysis to evaluate the efficiency of radiofrequency ablation (RFA) for the treatment of benign TNs in accord with the Preferred Reporting Items for Systematic Reviews and Meta-Analyses statements. Methods: Published literatures were retrieved from PubMed, Embase, Web of Science, and Scopus up to January 27, 2016.

Thyroid Radiofrequency Ablation Guideline: Korean Society of Thyroid Radiology
Thermal ablation using radiofrequency is a new, minimally invasive modality employed as an alternative to surgery in patients with benign thyroid nodules and recurrent thyroid cancers. The Task Force Committee of the Korean Society of Thyroid Radiology (KSThR) developed recommendations for the optimal use of radiofrequency ablation for thyroid tumors in 2012.

Long-term outcome of microwave ablation for benign thyroid nodules: Over 48-month follow-up study
The short-term effects of microwave ablation (MWA) for the treatment of benign thyroid nodules (BTNs) were satisfactory in previous studies. However, as a slowly progressing disease, the long-term efficacy of MWA for BTNs at present is not clear.

Update on Molecular Testing for Cytologically Indeterminate Thyroid Nodules. Archives of pathology & laboratory medicine
Context: Approximately 15% to 30% of thyroid nodules that undergo fine-needle aspiration are classified as cytologically indeterminate, presenting management challenges for patients and clinicians alike. During the past several years, several molecular tests have been developed to reduce the diagnostic uncertainty of indeterminate thyroid fine-needle aspirations. Objective: To review the methodology, clinical validation, and recent peer-reviewed literature for 4 molecular tests that are currently marketed for cytologically indeterminate thyroid fine-needle aspiration specimens: Afirma, ThyroSeq, ThyGenX/ThyraMIR, and RosettaGX Reveal.

Safety of radiofrequency ablation of benign thyroid nodules and recurrent thyroid cancers: a systematic review and meta-analysis
We performed a systematic review and meta-analysis to evaluate the safety of radiofrequency ablation (RFA) for the treatment of benign thyroid nodules and recurrent thyroid cancers

Radiofrequency Ablation of Benign Symptomatic Thyroid Nodules: Prospective Safety and Efficacy Study
Radiofrequency ablation (RFA) is a relatively novel procedure in the management of benign nodular goiter. This study was conducted to evaluate the safety and efficacy of ultrasound (US)-guided percutaneous RFA for benign symptomatic thyroid nodules as an alternative to surgery. Methods The study involved patients for whom a fine needle aspiration biopsy had proved a diagnosis of benign nodular goiter and had nodule-related symptoms such as dysphagia, cosmetic problems, sensation of foreign body in the neck, hyperthyroidism due to autonomous nodules or fear of malignancy.

For Percutaneous Radiofrequency Ablation of Thyroid Nodules
On December 9, 2024 the Centers for Medicare & Medicaid Services (CMS) released the CY 2025 MPFS Final Rule. In this rule, CMS finalized the valuation and established the official CPT code for percutaneous radiofrequency ablation of the thyroid.

Analyzing the adoption of radiofrequency ablation of thyroid nodules using the diffusion of innovations theory: understanding where we are in the United States?
Thyroid nodules are very common and found in up to 68% of the general U.S. population on ultrasound.

Radiofrequency Ablation of Solid, Non-Functional Thyroid Nodules
Thyroid RFA provides a minimally invasive, low risk, efficacious therapy for the treatment of this condition. Thyroid RFA enjoys similar efficacy as surgery, results in similar degrees of patient satisfaction, but does so with a lower risk profile.1,2 While many interventional radiologists will be familiar with thermal ablation in other organs, such as lung, liver, and kidneys, there are some important procedural modifications (namely the “moving shot” technique) which are unique to the neck.

Radiofrequency ablation and related ultrasound-guided ablation technologies for treatment of benign and malignant thyroid disease
The use of ultrasound-guided ablation procedures to treat both benign and malignant thyroid conditions is gaining increasing interest. This document has been developed as an international interdisciplinary evidence-based statement with a primary focus on radiofrequency ablation and is intended to serve as a manual for best practice application of ablation technologies. Methods: A comprehensive literature review was conducted to guide statement development and generation of best practice recommendations.

Ultrasound-guided percutaneous radiofrequency ablation for benign thyroid nodules. Interventional procedures guidance
Ultrasound-guided percutaneous radiofrequency ablation for benign thyroid nodules is safe enough and works well enough for use in the NHS. Before this procedure is used, the thyroid nodule must be tested to make sure it is benign (not cancerous). A thin needle is used to take a sample of tissue from the nodule, to check for cancer cells.

Contemporary Thyroid Nodule Evaluation and Management
Context: Approximately 60% of adults harbor 1 or more thyroid nodules. The possibility of cancer is the overriding concern, but only about 5% prove to be malignant.

Thyroid nodules treated with percutaneous radiofrequency thermal ablation: a comparative study
Percutaneous radiofrequency thermal ablation (RTA) was reported as an effective tool for the management of thyroid nodules (TNs). The aim of this study was to investigate the effects of RTA and to establish whether they were treatment-related by comparison with a matched, untreated control group.

Monopolar Radiofrequency Ablation of Thyroid Nodules: A Prospective Austrian Single-Center Study
Background: Monopolar radiofrequency ablation is currently deemed an exotic treatment option for benign thyroid nodules in many central European countries. The aim of this study was to evaluate prospectively the safety and efficacy of this method in a large patient cohort following its introduction in Austria. Methods: Peri- and post-interventional complications were analyzed for 277 patients.

Efficacy and Safety of Radiofrequency Ablation Versus Observation for Nonfunctioning Benign Thyroid Nodules: A Randomized Controlled International Collaborative Trial
Background: Percutaneous radiofrequency thermal ablation (RFA) has been reported as an effective tool for the management of benign thyroid nodules (BTN). However, large, randomized controlled trials (RCTs) are lacking. Objective: The aims of this study were to assess the volume reduction of BTN after a single RFA performed using the moving-shot technique and to compare the volume reduction obtained in patients treated in two centers with different experience of the moving-shot technique. Method: This study was an international prospective RCT.

Update of Radiofrequency Ablation for Treating Benign and Malignant Thyroid Nodules. The Future Is Now
Thermal and chemical ablation are minimally invasive procedures that avoid removal of the thyroid gland and target symptomatic nodules directly. Internationally, Radiofrequency ablation (RFA) is among one of the most widely used thermal ablative techniques, and is gaining traction in North America.

Outcomes of Radiofrequency Ablation Therapy for Large Benign Thyroid Nodules: A Mayo Clinic Case Series
Objective: To assess the effectiveness, tolerability, and complications of radiofrequency ablation (RFA) in patients with benign large thyroid nodules (TNs). Patients and methods: This is a retrospective review of 14 patients with predominantly solid TNs treated with RFA at Mayo Clinic in Rochester, Minnesota, from December 1, 2013, through October 30, 2016. All the patients declined surgery or were poor surgical candidates.

Safety and Efficacy of Radiofrequency Ablation of Thyroid Nodules—Expanding Treatment Options in the United States
Radiofrequency ablation (RFA) has only recently gained popularity in the United States for treatment of thyroid nodules (TNs), with a limited number of patients having undergone the procedure in this country. Objective: To evaluate the safety and efficacy of RFA of TNs performed in an outpatient setting in the United States. Methods: This is a retrospective, single-center study of 53 patients who underwent RFA of 58 TNs between November 2018 and January 2021. The reduction in volume of nodule, cosmetic and symptomatic improvement, effect on thyroid function, and complications following RFA were assessed. Results: Eleven out of 53 patients were excluded from the analysis.

Radiofrequency ablation and thyroid nodules: updated systematic review
In the thyroid gland, radiofrequency ablation (RFA) is being applied to both benign nodules and cancers internationally, while interest is also growing in the West. Benign thyroid nodules (BTNs) may be candidates for intervention when symptoms develop.

Radiofrequency Ablation for Autonomously Functioning Thyroid Nodules: A Multicenter Study
The purpose of this study is to validate the generalizability of the efficacy and safety of radiofrequency (RF) ablation for treating autonomously functioning thyroid nodules (AFTN) in a large population multicenter study. Methods: This study included 44 patients from 5 institutions who refused or were not suitable for surgery or radioiodine therapy.

Guidelines for Clinical Practice for the Diagnosis and Management of Thyroid Nodules – 2016 Update
Thyroid nodules are detected in up to 50 to 60% of healthy subjects. Most nodules do not cause clinically significant symptoms, and as a result, the main challenge in their management is to rule out malignancy, with ultrasonography (US) and fine-needle aspiration (FNA) biopsy serving as diagnostic cornerstones.

Radiofrequency Ablation for the Management of Thyroid Nodules: A Critical Appraisal of the Literature
The majority of benign thyroid nodules are asymptomatic, remain stable in size and do not require treatment. However, a minority of patients with growing nodules may have local symptoms or cosmetic concerns, and thus demand surgical therapy.

Long-Term Results of Ultrasound-Guided Radiofrequency Ablation of Benign Thyroid Nodules: State of the Art and Future Perspectives-A Systematic Review
Background: Nearly 20 years after the first feasibility study, minimally invasive ultrasound (US)-guided therapeutic techniques are now considered as a safe and effective alternative to surgery for symptomatic benign thyroid nodules. Radiofrequency ablation (RFA) is one of the most widely used treatment in specialized thyroid centers but, due to the relatively recent introduction into clinical practice, there are limited long-term follow-up studies.

Laser Ablation Versus Radiofrequency Ablation for Thyroid Nodules: 12-Month Results of a Randomized Trial (LARA II Study)
Radiofrequency ablation (RFA) seems to achieve a significantly larger nodule volume reduction rate (VRR) than laser ablation (LA) in benign nonfunctioning thyroid nodules (BNTNs). Objective: To compare the efficacy and safety of both treatments at 12-month follow-up in patients with solid or predominantly solid BNTN. Methods: This was a single-center, 12-month, randomized, superiority, open-label, parallel-group trial conducted in an outpatient clinic. Sixty patients with a solitary BNTN or dominant nodule characterized by pressure symptoms/cosmetic problems were randomly assigned (1:1 ratio) to receive either a single session of RFA or LA.

Thyroid Radiofrequency Ablation: Updates on Innovative Devices and Techniques
Radiofrequency ablation (RFA) is a well-known, effective, and safe method for treating benign thyroid nodules and recurrent thyroid cancers. Thyroid-dedicated devices and basic techniques for thyroid RFA were introduced by the Korean Society of Thyroid Radiology (KSThR) in 2012.

Radiofrequency Ablation of Cervical Thyroid Cancer Metastases—Experience of Endocrinology Practices in the United States
Radiofrequency ablation (RFA) is used in the United States to treat benign thyroid nodules; however, experience with treating cervical recurrence/persistence of papillary thyroid cancer (PTC) is limited. Objective To evaluate the efficacy RFA for the treatment of cervical recurrence/persistence of PTC in the United States. Although it is well recognized that surgery is the treatment of choice for recurrent thyroid cancer in the neck, some patients are not surgical candidates, or may not want to undergo repeat surgeries after their initial resection. While active surveillance is an option for selected patients, many patients have anxiety with this approach and may choose intervention despite no progression in tumor kinetics or size [30, 31].

Radiofrequency ablation for benign thyroid nodules
Benign thyroid nodules are an extremely common occurrence. Radiofrequency ablation (RFA) is gaining ground as an effective technique for their treatment, in case they become symptomatic.
The American Association of Endocrine Surgeons Guidelines for the Definitive Surgical Management of Thyroid Disease in Adults
Objective: To develop evidence-based recommendations for safe, effective, and appropriate thyroidectomy. Background: Surgical management of thyroid disease has evolved considerably over several decades leading to variability in rendered care. Over 100,000 thyroid operations are performed annually in the US. Methods: The medical literature from 1/1/1985 to 11/9/2018 was reviewed by a panel of 19 experts in thyroid disorders representing multiple disciplines.

Prospective validation of an ultrasound-based thyroid imaging reporting and data system (TI-RADS) on 3980 thyroid nodules
Ultrasound (US) features of solidity, hypoechogenicity or marked hypoechogenicity, microlobulated or irregular margins, microcalcifications, and taller-than-wide shape are suspicious characteristics for thyroid nodules. An US based Thyroid Imaging Reporting and Data System (TI-RADS) is classified based on the number of aforesaid features.

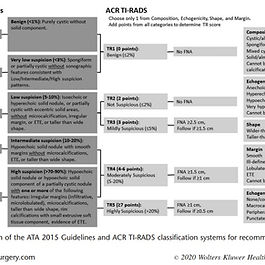
Tessler, F. N., Middleton, W. D., & Grant, E. G. (2018). Thyroid Imaging Reporting and Data System (TI-RADS): A User’s Guide.
In 2017, the Thyroid Imaging Reporting and Data System (TI-RADS) Committee of the American College of Radiology (ACR) published a white paper that presented a new risk-stratification system for classifying thyroid nodules on the basis of their appearance at ultrasonography (US). In ACR TI-RADS, points in five feature categories are summed to determine a risk level from TR1 to TR5.

Radiofrequency Ablation Compared to Surgery for the Treatment of Benign Thyroid Nodules
Objective Benign thyroid nodules are a common occurrence whose only remedy, in case of symptoms, has always been surgery until the advent of new techniques, such as radiofrequency ablation (RFA). This study aimed at evaluating RFA efficacy, tolerability, and costs and comparing them to hemithyroidectomy for the treatment of benign thyroid nodules.

RFA and benign thyroid nodules: Review of the current literature
Benign thyroid nodules (BTNs) are commonly found in the general population. They are usually asymptomatic and their incidence has increased as a result of wide‐spread use of ultrasound.

Radiofrequency ablation of benign thyroid nodules: safety and imaging follow-up in 236 patients
This study evaluated the safety and volume reduction of ultrasonography (US)-guided radiofrequency ablation (RFA) for benign thyroid nodules, and the factors affecting the results obtained. A total of 302 benign thyroid nodules in 236 euthyroid patients underwent RFA between June 2002 and January 2005.
Microwave ablation (MWA) for thyroid nodules: a new string to the bow for percutaneous treatments?
Thyroid nodules are a fairly common finding in general population and, even if most of them are benign, a treatment can be however necessary. In the last years, non surgical minimally invasive techniques have been developed to treat this pathology, starting from percutaneous ethanol injection (PEI), to laser ablation (LA), radiofrequency ablation (RFA) and, most recently, microwave ablation (MWA). Most recently, microwave ablation (MWA) has been proposed to treat thyroid nodules, taking experience from its use in other organs like liver, kidney and lung in particular (9).

Radiofrequency Ablation of Indeterminate Thyroid Nodules: The First North American Comparative Analysis
Thyroid nodules can be classified as benign, malignant, or indeterminate, the latter of which make up 10–30% of nodules. Radiofrequency ablation (RFA) has become an attractive and promising therapy for the treatment of benign thyroid nodules.

Radiofrequency ablation for benign thyroid nodules: 450 patients - three years follow-up
Purpose: The objective of this study was to evaluate the efficacy and safety of ultrasound (US)-guided radiofrequency ablation (RFA) for treating of benign thyroid nodules. Material and methods: The retrospective analysis included the results of treatment of 450 patients with benign tumors of the thyroid gland in the Samara Oncology Center. 91 (20.2%) patients had autonomously functioning thyroid nodules and 359 (79.8%) had symptomatic ones.

Conventional thyroidectomy vs thyroid thermal ablation on postoperative quality of life and satisfaction for patients with benign thyroid nodules
The complications and treatment effects of conventional thyroidectomy and thyroid thermal ablation should be compared in order to identify the best intervention for patients with benign thyroid nodules.

Efficacy of radiofrequency ablation in autonomous functioning thyroid nodules. A systematic review and meta-analysis
Whether thermal ablation is effective to treat toxic thyroid nodules (TTN) is still unknown. Aim of this review was to achieve more robust evidence on the efficacy of radiofrequency ablation (RFA) in treating TTN in terms of TSH normalization, thyroid scintiscan, and volume reduction rate (VRR).

RFA of thyroid nodules: Good Clinical Practice Recommendations for Austria
The present "Good Clinical Practice Recommendations" relate to radiofrequency ablation (RFA) training, execution, and quality control, as well as to pre- and postinterventional standards of care. They are aimed at all physicians who intend to learn to perform, or who are already conducting RFA interventions as well as at thyroid specialists providing pre- and postoperative care to RFA patients in Austria.

A Propensity-Matched Cohort Study
BACKGROUND AND PURPOSE: Ultrasound-guided radiofrequency ablation has been recommended as an alternative to surgery for benign thyroid nodules. However, little is known about the benefit from the application of radiofrequency ablation for benign thyroid nodules in elderly patients.

Radiofrequency ablation, cryoablation, irreversible electroporation, and other ablation procedures.
David Zielske, MD, CIRCC, COC, CCVTC, CCC, CCS, RCC, is the founder and President of ZHealth Publishing. As the primary author and editor of each ZHealth publication, "Dr.

Choice in Ablative Therapies for Thyroid Nodules
Ultrasound-guided ablation procedures have been growing in popularity and offer many advantages compared with traditional surgery for thyroid nodules. Many technologies are available, with thermal ablative techniques being the most popular currently though other nonthermal techniques, such as cryoablation and electroporation, are gaining interest.

Insurance Authorization Letter for Radiofrequency Ablation of the Thyroid Gland
Currently the evaluation of the thyroid nodules is covered by insurance companies. However, radiofrequency ablation of thyroid nodules is new and is not considered a recognized benefit.

Radiofrequency ablation for thyroid nodules: which indications? The first Italian opinion statement
Nodular thyroid disease is a very common finding in clinical practice, discovered by ultrasound (US) in about 50 % of the general population, with higher prevalence in women and in the elderly [1–4]. Whereas therapeutic flowchart is quite established and shared for malignant lesions, multiple options are now available for patients presenting with benign thyroid nodules, ranging from simple clinical and US follow-up to thyroid surgery. The majority of thyroid nodules, benign by fine-needle aspiration, are asymptomatic, stable, or slow-growing over time and require no treatment. Nevertheless, large thyroid nodules may become responsible for pressure symptoms, resulting in neck discomfort, cosmetic complaints, and decreased quality of life.

Recommendations from the Asian Conference on Tumor Ablation Task Force – Secondary Publication
Radiofrequency ablation (RFA) is a thermal ablation technique widely used for the management of benign thyroid nodules. To date, five academic societies in various countries have reported clinical practice guidelines, opinion statements, or recommendations regarding the use of thyroid RFA.

Microwave ablation of benign thyroid nodules
Microwave ablation (MWA) has become increasingly popular as a minimally invasive treatment for benign and malignant tumors of the liver, lung and kidney. Recently, two studies have attempted to apply the technique to debulk benign thyroid nodules and gained positive results.

Microwave ablation of thyroid nodules and metastatic thyroid cervical lymph nodes: the first case series from Ecuador
Microwave ablation (MWA) has emerged as a minimally invasive technique, transforming the therapeutic landscape for benign thyroid nodules (BTN), papillary thyroid microcarcinoma (PTMC), and cervical lymph node metastasis (CLNM). This study aims to present the first experience in Ecuador using MWA.

Clinical Utility of Minimally Invasive Interventional Procedures in the Management of Benign and Malignant Thyroid Lesions
The objective of this disease state clinical review is to provide clinicians with a summary of the nonsurgical, minimally invasive approaches to managing thyroid nodules/malignancy, including their indications, efficacy, side effects, and outcomes.

Novel Approaches for Treating Autonomously Functioning Thyroid Nodules
Benign thyroid nodules are exceedingly common in the adult population. Only a small percentage of nodules are toxic or autonomously functioning thyroid nodules (AFTNs).
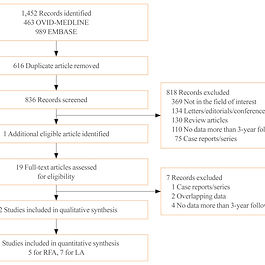
Long-Term Results of Thermal Ablation of Benign Thyroid Nodules: A Systematic Review and Meta-Analysis
Background: Ultrasound-guided thermal ablations have become one of the main options for treating benign thyroid nodules. To determine efficacy of thermal ablation of benign thyroid nodules, we performed a meta-analysis of studies with long-term follow-up of more than 3 years. Methods: Databases were searched for studies published up to August 25, 2019, reporting patients with benign thyroid nodules treated with thermal ablation and with follow-up data of more than 3 years.

Efficacy of thermal ablation in benign non-functioning solid thyroid nodule: A systematic review and meta-analysis
Image-guided thermal ablations are commonly used in the treatment of thyroid nodules. Radiofrequency ablation (RFA) and laser ablation are the most commonly used.

General Principles for the Safe Performance, Training, and Adoption of Ablation Techniques for Benign Thyroid Nodules: An American Thyroid Association Statement
Background: The primary goal of this interdisciplinary consensus statement is to provide a framework for the safe adoption and implementation of ablation technologies for benign thyroid nodules. This consensus statement is organized around three key themes: (1) safety of ablation techniques and their implementation, (2) optimal skillset criteria for proceduralists performing ablative procedures, and (3) defining expectations of success for this treatment option given its unique risks and benefits. Ablation safety considerations in pre-procedural, peri-procedural, and post-procedural settings are discussed, including clinical factors related to patient selection and counseling, anesthetic and technical considerations to optimize patient safety, peri-procedural risk mitigation strategies, post-procedural complication management, and safe follow-up practices.

Guidelines for Adult Patients with Thyroid Nodules and Differentiated Thyroid Cancer 2015
Background: Thyroid nodules are a common clinical problem, and differentiated thyroid cancer is becoming increasingly prevalent. Since the American Thyroid Association's (ATA's) guidelines for the management of these disorders were revised in 2009, significant scientific advances have occurred in the field.

Interventional procedure overview of ultrasound-guided percutaneous radiofrequency ablation for benign thyroid nodules
Thyroid nodules are lumps in the thyroid gland. The majority are benign (not cancerous) and this must be determined using appropriate diagnostic tests.

Predictor Analysis in Radiofrequency Ablation of Benign Thyroid Nodules: A Single Center Experience
Purpose: To confirm the efficacy of ultrasound (US) guided radiofrequency ablation (RFA) in the treatment of benign thyroid nodules, we evaluated as primary outcome the technical efficacy and clinical success in a single center dataset. The secondary outcome was to find a correlation between nodules’ pre-treatment features and volume reduction rate (VRR) ≥75% at 12 months after RFA and during follow-up period. Methods: This retrospective study included 119 consecutive patients (99 females, 20 males, 51.5 ± 14.4 years) with benign thyroid nodules treated in our hospital between October 2014 and December 2018 with a mean follow-up of 26.8 months (range 3–48).

